IntroductionIn order to make sense of the joint examination, you must have an understanding of functional anatomy. Without this, the provocative maneuvers used to define the precise nature of the joint problem will make no sense. By gaining an appreciation for the basic structures and functioning of the joint, you’ll be able to “logic” your way thru the exam, even if you can’t remember the eponym attached to each specific test! The complete examination of the knee or shoulder is usually performed in the setting of pain, decline in function or other focal complaint. |
||||||||||||
|
|
||||||||||||
Shoulder ExamI think that the most daunting aspect of the shoulder exam is appreciating Observation The shoulder joint is created by the confluence of 3 bony structures: the scapula,
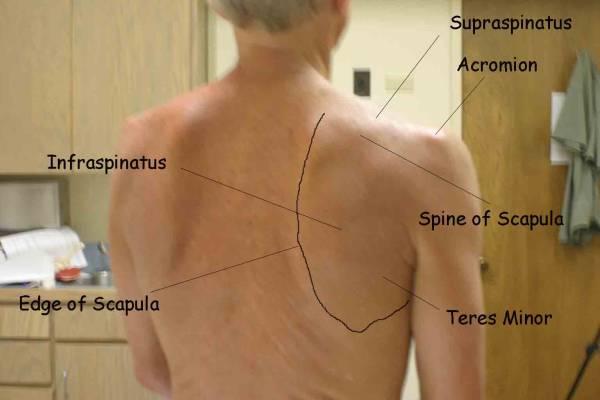
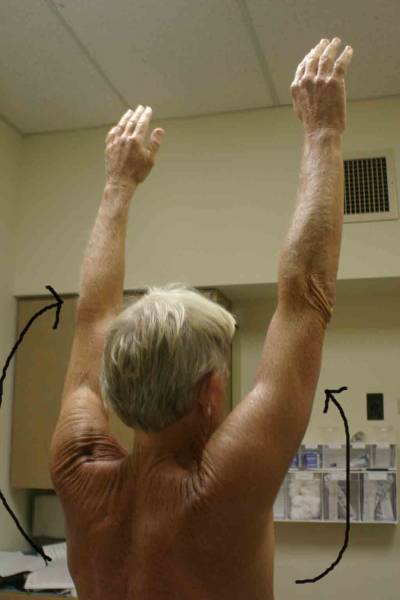
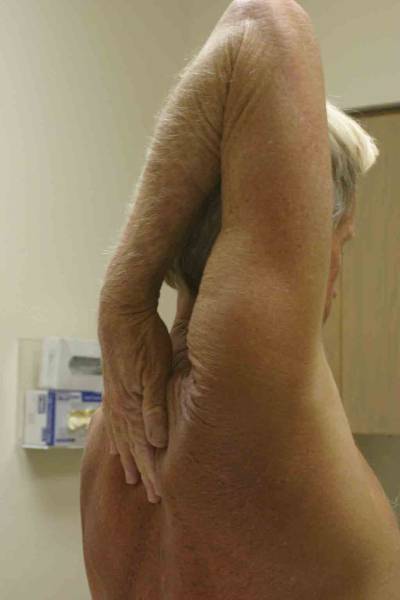
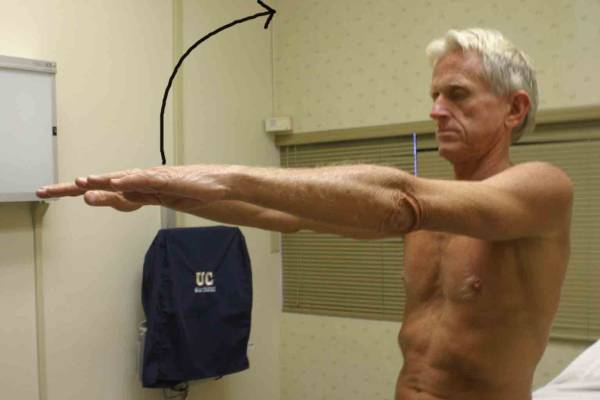
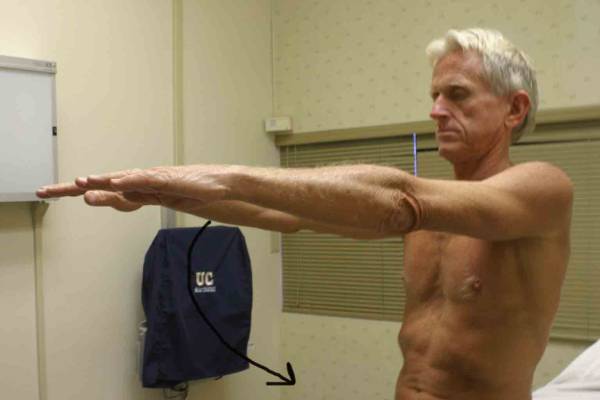
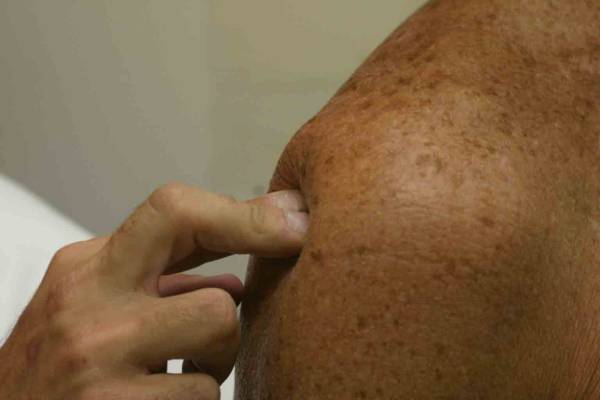
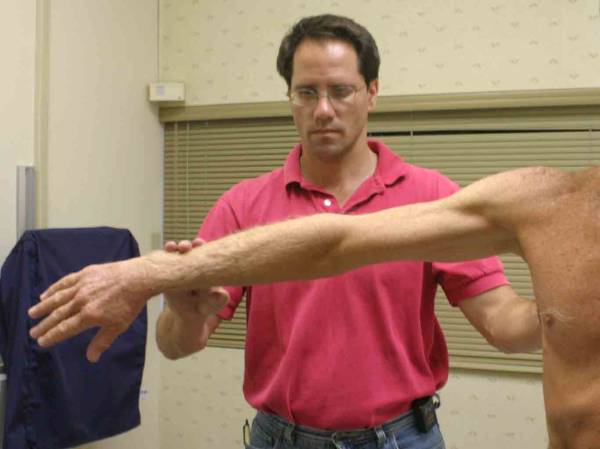
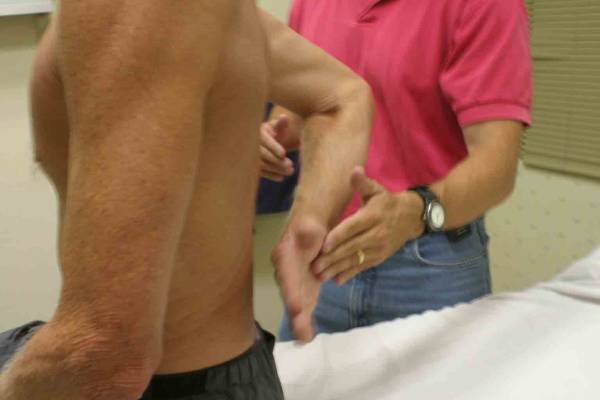
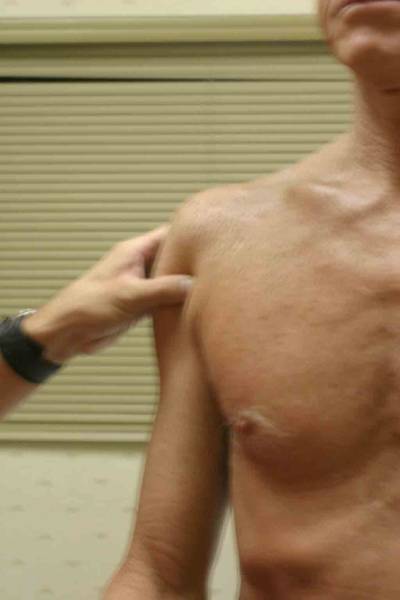
Location Of The Muscle Groups Is Approximated In The Pictures Above. Start by looking at the normal (or more normal) side. Note any scars, Palpation Gently palpate around the shoulder, touching each of the Range of Motion (ROM) If there are no symptoms, test both sides simultaneously. Otherwise, start Active ROM:
Passive ROM If there is pain with active ROM, assess the same movements with passive ROM. Pain/limitation on active ROM but not present with passive suggests |
||||||||||||
|
|
||||||||||||
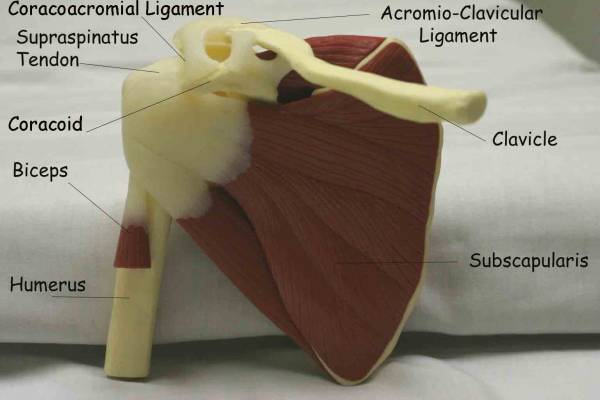
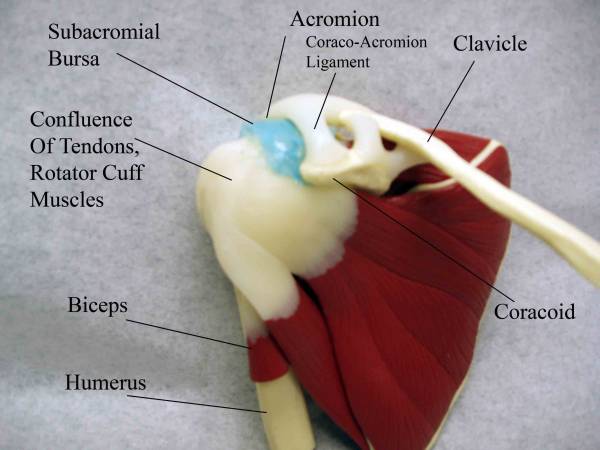
Impingement, Rotator Cuff Tendonitis and Sub-Acromial BursitisAnatomy and Function: I have placed these processes under one heading Right Shoulder Anatomy (anterior view) Several tests can be done to localize the problem: Sub-acromial Palpation: Gently palpate in the region of the sub-acromial The following two tests passively maneuver the tendons so that they are most Neers Test:
Neer’s Test For Impingement Hawkin’s (for more subtle impingement)
Hawkins Test For Impingement
It’s worth noting that defining the precise location of the problem (ie. bursitis, |
||||||||||||
|
|
||||||||||||
Evaluation of the Muscles of the Rotator CuffAnatomy and Function: There are 4 major muscles that allow shoulder Supraspinatus: Connects the top of the scapula to the humerus. Contraction
Supraspinatus (Empty Can)Test Interpretation: If there is a partial tear of the muscle or tendon, the patient Infraspinatus: Connects the scapula to the humerus. Contraction allows
Interpretation: Tears in the muscle will cause weakness and/or pain. Testing Infraspinatus And Teres Minor (External Rotators) Teres Minor: Connects the scapula to the humerus. Provides the same Subscapularis: Connects the scapula to the humerus, though the origin
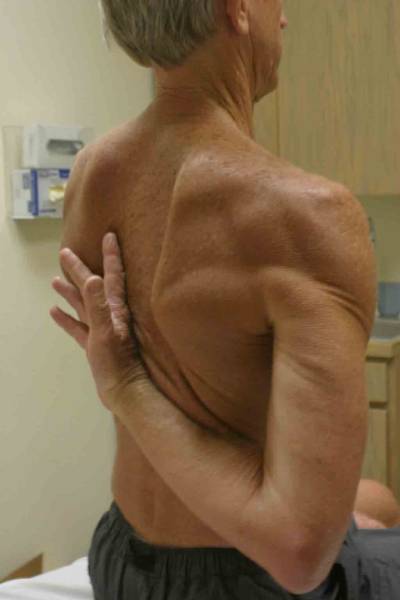
Gerbers Liftoff Test (Subscapularis)
Drop Arm Test for Supraspinatus Tears: Adducting the arm depends upon
Deltoid: Not a muscle of the rotator cuff, but important for the later
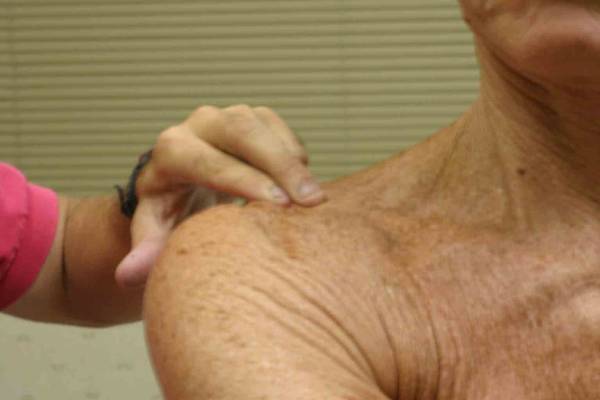
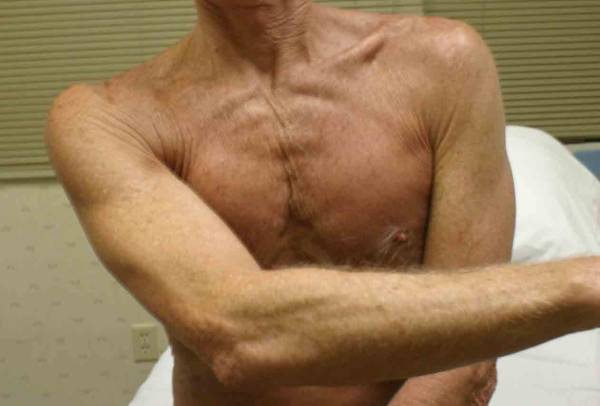
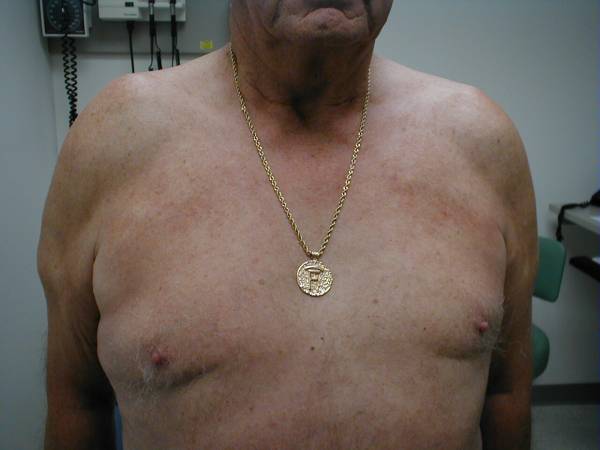
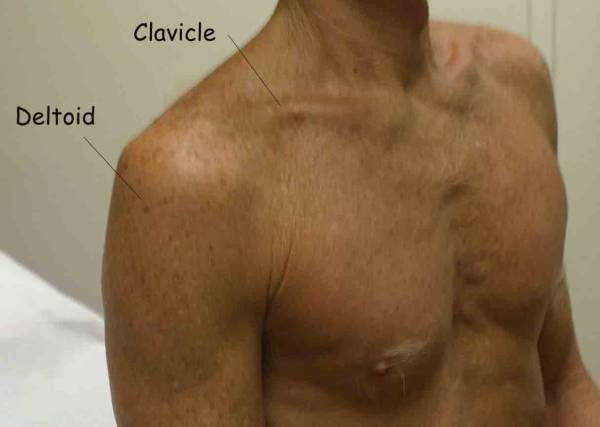 Acromioclaviular Arthritis Anatomy and Function: The A-C joint is minimally
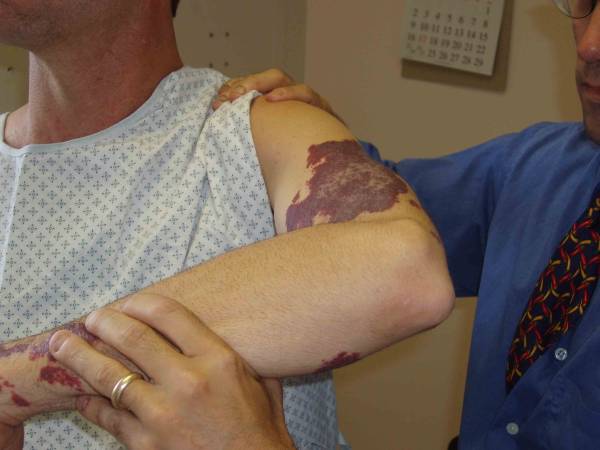
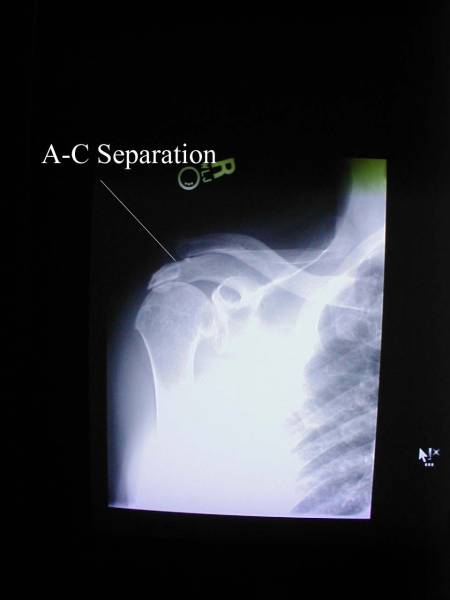
AC Disruption: Trauma can cause disruption of the ac joint, also known
|
||||||||||||
|
|
||||||||||||
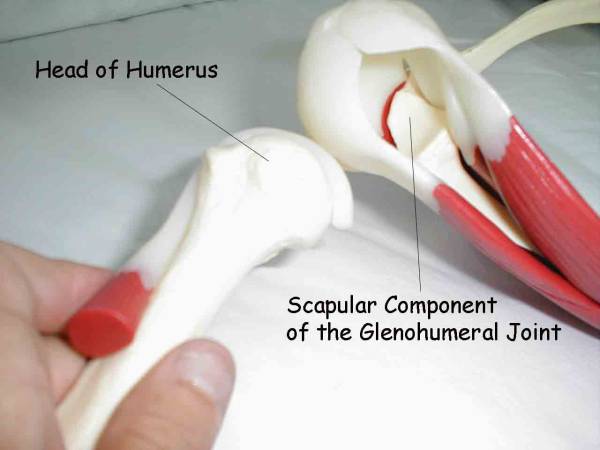
The Glenohumeral JointAnatomy and Function: This joint is the actual place where the humerus Glenohumeral DJD: DJD usually results from an injury that has disrupted
Glenohumeral Joint Anatomy-Humerus has been removed from
Glenohumeral Instability: The rotator cuff, along with the outer
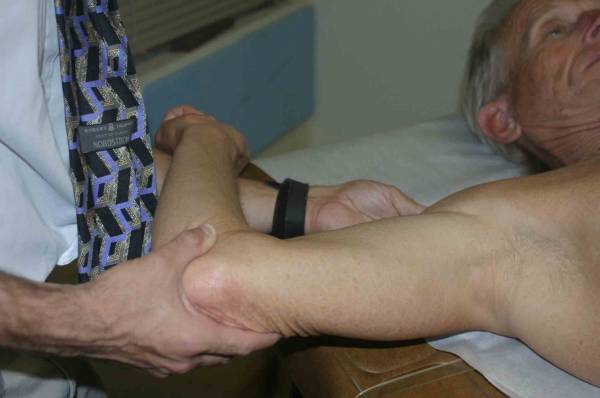
Testing Glenohumeral Stability Acute Inflammatory Arthritis: Inflammatory processes within the joint
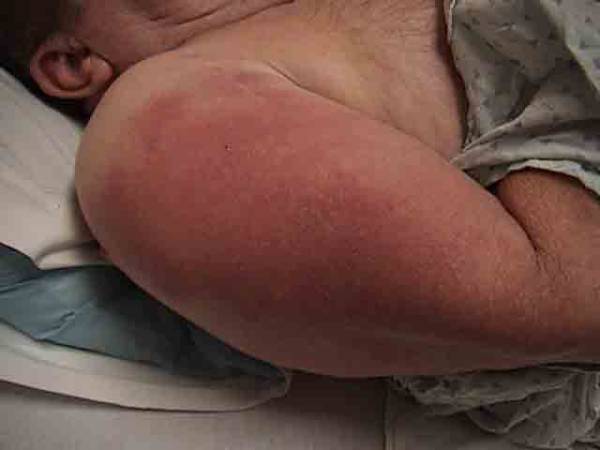
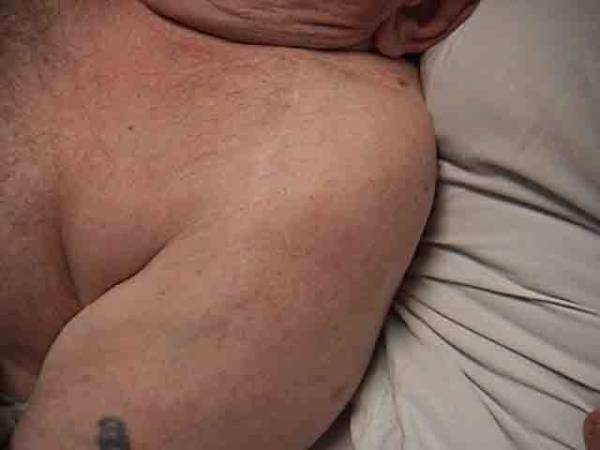
Septic Shoulder: Intense Inflammation Over Shoulder Area As Seen In Picture On Right Is Normal For Comparison.
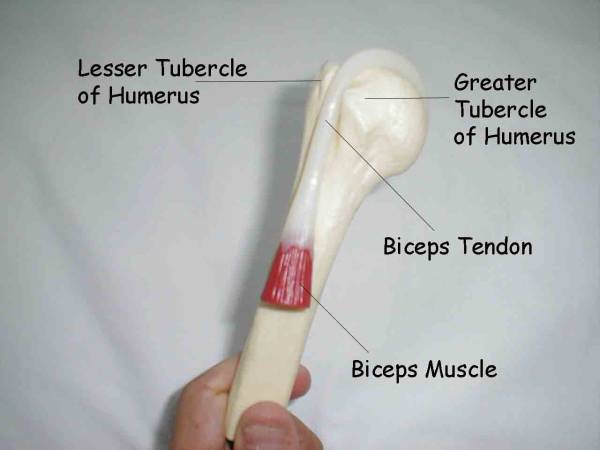
Biceps Tendonitis: The long head of the biceps tendon inserts on the
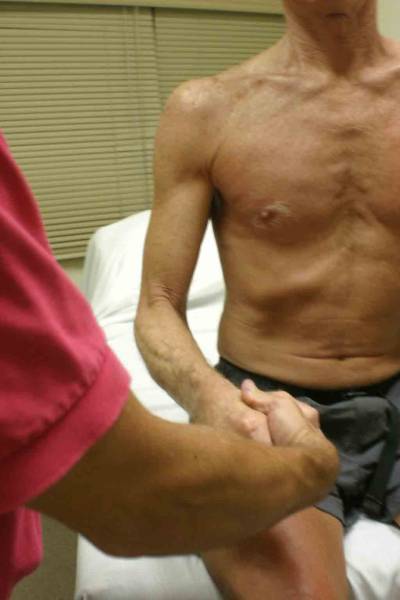
Resisted Supination (Yergason’s Test):
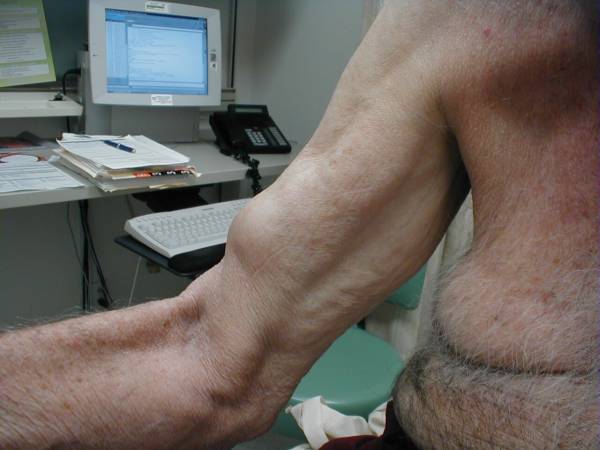
Resisted Supination (Yergason’s Test) Biceps Tendon Rupture: As a result of chronic tendonitis or truama, Balled Up Biceps Secondary to Tendon Rupture Adhesive Capsulitis: Also called a frozen shoulder, this is caused by |
||||||||||||
|
|
||||||||||||
Referred Pain to the Shoulder AreaIt’s important to recognize that not all shoulder pain is cause by shoulder
|
||||||||||||
|
|
||||||||||||
| Adapted, with permission from University of California, San Diego School of Medicine By Charlie Goldberg, M.D. | ||||||||||||
|
|
||||||||||||
| Jump to: Top of the Page | ||||||||||||